Caesarean section is considered the most common surgical procedure performed by obstetricians. This surgery can effectively prevent maternal and neonatal mortality when performed for medical reasons.
Globally, caesarean section rates have increased over the past decades.
According to recent estimates covering 150 countries, 21% of all births are by caesarean section, with averages ranging from 1% to 58% depending on the country. According to WHO estimates, the global caesarean section rate has almost tripled in a quarter of a century, from 6.7% in 1990 to 19.1% in 2014.
In France, the predominant role of midwives in the follow-up of pregnant women, education and preparation sessions for childbirth and the systematic review of the indications for scheduled caesarean sections by peers have made it possible to stabilise the caesarean section rate at around 20% since the early 2000s(1,2).
Abdominal/pelvic adhesions are fibrous bands (sort of rigid cobwebs) that form between the abdominal organs or between the peritoneum and the abdominal wall and occur immediately after surgery in a completely unpredictable way.
The reported incidence of adhesion development after a first caesarean section varies from 46 to 65%. The density of adhesions can vary considerably and their size and location are likely to influence the clinical effects. Adhesions are particularly thick and dense after several caesarean sections.
In a retrospective study of 542 patients, it was shown that the percentage of women with adhesions increases with each caesarean section(2).

Intra-abdominal adhesions can complicate surgical procedures and prolong their duration, increasing the risk of infection and blood loss. They can disrupt a delivery in the case of emergency caesarean and cause later complications such as infertility, bowel obstruction or chronic pelvic pain(3).
Wound healing and adhesion formation are processes controlled by inflammatory, hormonal and genetic factors and therefore depend on each individual. There is an association between scarring problems – such as keloids – and dense intra-abdominal adhesions. A very recent study showed that women with severe stretch marks had thick intraperitoneal adhesions. Women with intraperitoneal adhesions had more vascular, hyperpigmented, less flexible and hypertrophic scars(4) confirming that these adhesions occur in people with healing defects(3).
There is no single, validated and standardised method to assess and describe intra-abdominal adhesions. Researchers have used different scoring systems which remain complicated. Adhesions can be assessed based on location, severity (fragile to cohesive), extent, involvement of adjacent organs such as the bladder, bowel and omentum (fatty tissue that covers the organs in the abdomen, the peritoneum(3).
Treatment options for C-section scars include non-surgical methods: pressotherapy, local drug injection, IPL and therapeutic laser.
These treatments partially improve the appearance and pruritus but not the depression caused by some scars.
Surgical treatment is also widely used and consists of cutting the scar along the original incision and releasing the adhesions between the subcutaneous fat and the abdominal wall muscle. However, these surgical treatments lead to a very high incidence of new adhesions and the formation of new scars.
Autologous fat grafting or lipofilling is often used to treat body contour defects. Fat indeed contains stem cells with remarkable
regenerative potential and the ability to restore damaged tissue. Fat is therefore able to affect wound healing, soft tissue restoration and scar remodeling(5).
In addition to its volumetric capacity, fat helps to stimulate the growth and quality of the skin and adjoining tissues.
The effectiveness of lipofilling combined with surgical treatment in the treatment of adhesions caused by caesarean section scars was evaluated in a recent study involving 36 patients.
All patients had a marked improvement in scar appearance, texture and depression during 12 months of follow-up. Scores for colour, pain, pruritus, hardness, mobility and scar appearance after lipofilling were significantly improved compared to pre-treatment scores.
None of the patients reported any serious adverse effects. Autologous fat transplantation combined with adhesion release can be a good treatment option for abdominal wall scars after caesarean section. This method is minimally invasive and effective in obtaining good functional and aesthetic results(5).
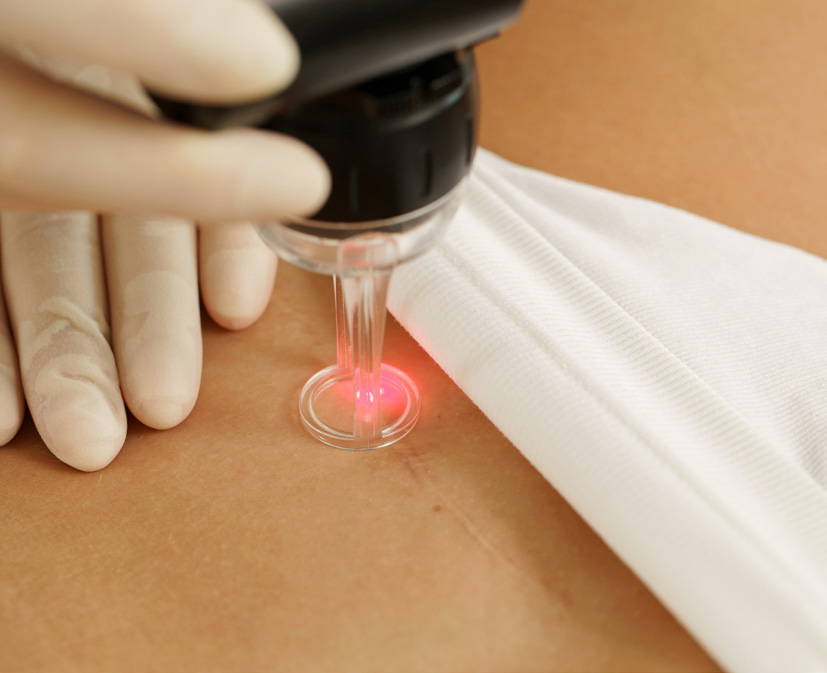
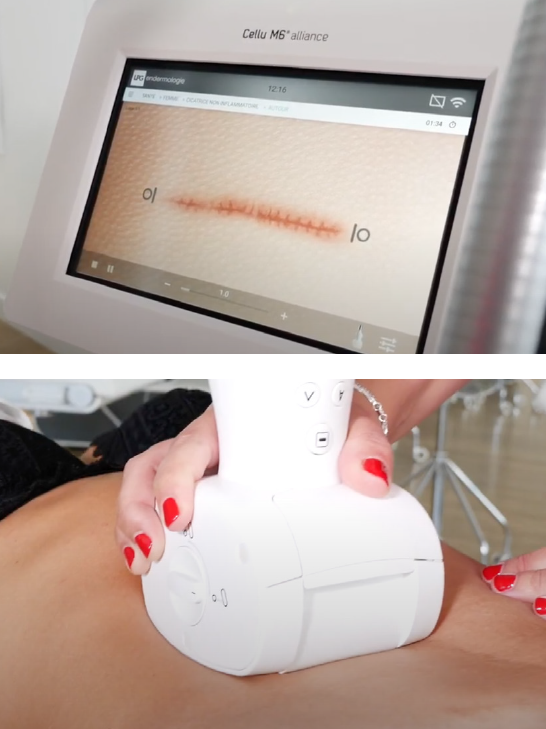
A more natural and non-invasive approach can be used with endermologie® treatments (LPG® technique), which treat recent or old scars, thanks to a painless mobilisation of tissues to regain good tissue flexibility and elasticity. They are particularly indicated in the treatment of adhesions. Many equipped physiotherapists obtain very good results on adherent scars of all origins.
These treatments are particularly recommended as a preventive measure for people who have healing defects and are likely to develop adhesions. The draining and defibrosing properties of the LPG® technique allow early and painless intervention on scars, preventing them from going down the wrong path with more or less disabling consequences in the medium and long term, not to mention the unsightly side.
SOURCES:
1. Dumont, Alexandre, et Christophe Z. Guilmoto. « Trop et pas assez à la fois : le double fardeau de la césarienne »,
Population & Sociétés, vol. 581, no. 9, 2020, pp. 1-4.
2. Lyell DJ. Adhesions and perioperative complications of repeat cesarean delivery. Am J Obstet Gynecol. 2011 Dec;205(6
Suppl):S11-8.
3. Herzberger EH et al. Adhesions at repeat cesarean delivery: is there a personal impact? Arch Gynecol Obstet. 2015
Oct;292(4):813-8.
4. Elprince M. et al. Prediction of intraperitoneal adhesions using striae gravidarum and scar characteristics
in women endergoing repeated cesarean sections. BMC Pregnancy Childbirth. 2021 Apr 9;21(1):286 (read here)
5. Li SH et al. Autologous fat transplantation for the treatment of abdominal wall
scar adhesions after cesarean section. J Plast Surg Hand Surg. 2021 Aug;55(4):210-215 (read here)




